I understand how frightening and disruptive Alpha-Gal Syndrome can be, especially when allergic reactions seem unpredictable and tied to foods you once tolerated without concern. Many of my patients come to me feeling confused, anxious, and unsure how to navigate their daily lives safely.
I want you to know that your symptoms are real, and there are clear, evidence-based steps we can take to uncover the root causes of your reactions. With a functional and integrative approach, I will help you regain confidence, reduce inflammation, and restore your quality of life.
-Dr. Dana Cohen
Sign-up today and receive ta FREE Dry Brushing Guide written by Dr. Dana Cohen
What Is Alpha-Gal Syndrome?
Alpha-Gal Syndrome is a delayed allergic reaction to a carbohydrate molecule called galactose‑alpha‑1,3‑galactose, commonly known as alpha‑gal. This molecule is found in the meat of mammals such as beef, pork, and lamb, as well as in certain products derived from mammals. The condition is most often triggered by a bite from the Lone Star tick, which introduces alpha-gal into the bloodstream and sensitizes the immune system.
Once sensitized, the body may react hours after consuming mammalian meat or related products. Symptoms can range from mild digestive discomfort to severe anaphylaxis. Because reactions are delayed, many patients struggle to identify the cause of their symptoms. Alpha‑Gal Syndrome is increasingly recognized across the United States, especially in regions where the Lone Star tick is expanding. Early diagnosis and personalized treatment are essential for preventing complications and improving long-term health.
Common Symptoms of Alpha-Gal Syndrome
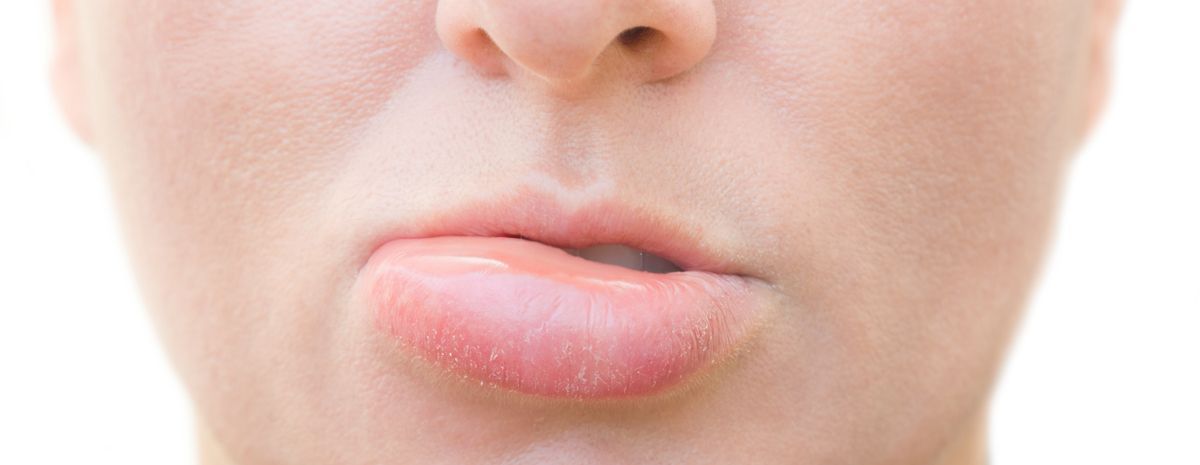
Swelling of the lips is a symptom of Alpha-Gal Syndrome
Many patients with Alpha‑Gal Syndrome experience symptoms that appear several hours after eating, making the condition difficult to identify. These symptoms can vary widely in severity and may affect multiple systems in the body. Understanding the full range of possible reactions helps guide accurate diagnosis and effective treatment.
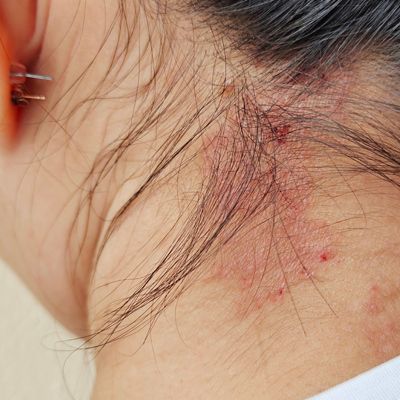
- Hives or skin rashes – These reactions often appear as raised, itchy welts that may spread across the body. They can occur several hours after eating mammalian meat, making the connection easy to miss.
- Gastrointestinal distress – Symptoms may include abdominal pain, nausea, vomiting, or diarrhea. These reactions can mimic food poisoning or irritable bowel syndrome, leading to misdiagnosis.
- Swelling of the lips, face, or throat – This swelling can be alarming and may progress quickly, especially in individuals with heightened sensitivity. It requires immediate medical attention if breathing becomes difficult.
- Respiratory symptoms – Patients may experience coughing, wheezing, or shortness of breath. These symptoms can resemble asthma or allergic reactions to airborne triggers.
- Dizziness or fainting – These symptoms may indicate a more severe allergic response that can affect blood pressure. They can occur suddenly and require urgent evaluation.
- Anaphylaxis – This is the most serious reaction and can be life-threatening. It may involve multiple systems and require emergency treatment.
These symptoms can be unpredictable and may worsen over time without proper diagnosis. Many patients struggle for months or years before discovering the underlying cause. With the right testing and integrative care, symptoms can be significantly reduced or eliminated.
Types of Alpha-Gal Syndrome
Alpha-Gal Syndrome can present in several forms depending on an individual’s immune response and sensitivity. Some patients experience primarily gastrointestinal symptoms, while others develop severe allergic reactions involving the skin or respiratory system. A subset of individuals may react not only to mammalian meat but also to dairy products, gelatin, or medications containing mammal-derived ingredients.
Another type involves reactions triggered by exercise or alcohol consumption shortly after eating mammalian foods, which can intensify the immune response. Some patients experience chronic inflammation and fatigue even when avoiding trigger foods. Others may have reactions only after repeated exposures, making the condition harder to detect.
There are also cases where symptoms improve over time, especially with reduced tick exposure and targeted treatment. Understanding the specific type of Alpha‑Gal Syndrome helps guide personalized care and long-term management.
Common Causes of Alpha-Gal Syndrome
Alpha‑Gal Syndrome is most commonly caused by the bite of the Lone Star tick, which introduces alpha‑gal into the bloodstream and triggers an immune response. The immune system then becomes sensitized, leading it to react to mammalian meat and related products. Environmental factors, such as living in wooded or grassy areas, increase the risk of tick exposure. Repeated tick bites can worsen sensitivity and prolong symptoms.
Some individuals may also develop reactions after exposure to medications or vaccines containing mammal-derived ingredients. Genetic predispositions may influence the severity of the immune response. Chronic inflammation and immune dysregulation can intensify symptoms. Understanding these causes helps guide prevention and long-term treatment strategies.
Candidates for Alpha-Gal Syndrome Treatment
Individuals who experience delayed allergic reactions after eating mammalian meat may be strong candidates for evaluation. Those with unexplained hives, swelling, or digestive issues should also consider testing for Alpha‑Gal Syndrome. Patients who have been bitten by ticks and later developed food sensitivities may benefit from an integrative assessment.
Anyone with chronic inflammation, fatigue, or immune dysregulation may find relief through functional medicine. Individuals who have seen multiple specialists without clear answers often benefit from a whole-body approach. Patients seeking natural, root‑cause-focused care are ideal candidates for integrative treatment. Those with overlapping conditions, such as MCAS or histamine intolerance, may also require specialized support. Early evaluation helps prevent complications and improve long-term health.
Related Conditions That Can Be Treated by Dr. Dana Cohen
Many patients with Alpha‑Gal Syndrome also experience other inflammatory or immune-related conditions. These conditions may overlap or share similar triggers, making integrative evaluation essential. Addressing these related issues can significantly improve overall health and symptom control.
- Mast Cell Activation Syndrome (MCAS) – This condition involves overactive mast cells that release excessive histamine and inflammatory chemicals. It can amplify allergic reactions and make Alpha‑Gal symptoms more severe.
- Chronic Inflammation – Persistent inflammation can weaken the immune system and increase sensitivity to allergens. Treating inflammation helps stabilize the body’s response to triggers.
- Food Sensitivities – Many patients develop sensitivities to dairy, gluten, or processed foods. Identifying and removing these triggers can reduce overall immune burden.
- Histamine Intolerance – This condition occurs when the body cannot effectively break down histamine. It can mimic or worsen Alpha‑Gal reactions.
- Gut Dysbiosis – Imbalances in gut bacteria can contribute to immune dysfunction and digestive symptoms. Restoring gut health supports long-term recovery.
These related conditions often overlap, complicating diagnosis. By addressing them together, patients experience more complete and lasting improvement. Integrative treatment helps restore balance across multiple systems, leading to better long-term outcomes.
How Conventional Medicine Treats Alpha-Gal Syndrome
Conventional medicine typically focuses on identifying the allergy through blood testing and recommending strict avoidance of mammalian meat. Patients may be prescribed antihistamines to manage mild reactions. In more severe cases, an epinephrine auto-injector is recommended for emergency use. Conventional care may also include education on reading food labels and avoiding hidden sources of alpha‑gal.
While these steps are essential, they often do not address underlying inflammation or immune dysregulation. Many patients continue to experience symptoms even with avoidance alone. Conventional medicine provides important safety measures but may not offer comprehensive long-term solutions. Integrating functional medicine can help fill these gaps.
How Traditional Medicine Treats Alpha-Gal Syndrome
Traditional medicine approaches Alpha‑Gal Syndrome by focusing on symptom management rather than root‑cause healing. Patients are advised to avoid mammalian meat and related products to prevent reactions. Antihistamines may be used to reduce itching, swelling, and mild allergic symptoms. Corticosteroids may be prescribed for more severe inflammatory responses.
Emergency medications such as epinephrine are recommended for individuals at risk of anaphylaxis. Traditional care may also include referrals to allergists for ongoing monitoring. While these treatments help manage acute symptoms, they do not address immune imbalances or chronic inflammation. Many patients benefit from a more holistic approach that supports long-term healing.
How Dr. Dana Cohen Treats Alpha-Gal Syndome with Functional and Integrative Medicine
My approach begins with a comprehensive evaluation of your immune system, inflammation levels, gut health, and environmental exposures. I use advanced testing to identify hidden triggers and assess the severity of your sensitivity. Treatment focuses on reducing inflammation, supporting detoxification pathways, and restoring immune balance. Dietary guidance is personalized to your specific sensitivities and nutritional needs.
I also incorporate targeted supplements to stabilize mast cells and reduce histamine overload. Gut‑healing protocols help strengthen the immune system and improve digestion. Lifestyle strategies, including stress reduction and sleep optimization, support long-term recovery. My goal is to help you regain confidence, reduce symptoms, and restore your quality of life.
Possible Side Effects of Treatment
Some patients may experience temporary changes in their digestion as their diet is adjusted. Mild fatigue can occur as the body detoxifies and inflammation decreases. Certain supplements may cause mild nausea if taken without food. Adjusting to new dietary restrictions may feel emotionally challenging at first. Rarely, patients may experience temporary symptom flare-ups as the immune system recalibrates. These effects typically resolve quickly with proper guidance and monitoring.
What Can Happen if Alpha-Gal Syndrome Is Left Untreated?
If Alpha‑Gal Syndrome is left untreated, symptoms may worsen over time and become more unpredictable. Repeated exposures to mammalian meat can increase the risk of severe allergic reactions, including anaphylaxis. Chronic inflammation may develop, affecting multiple systems in the body. Digestive issues may become more frequent and harder to manage.
Patients may experience ongoing fatigue and reduced quality of life. Untreated Alpha‑Gal Syndrome can also contribute to anxiety around food and social situations. Over time, immune dysregulation may lead to additional sensitivities. Early diagnosis and treatment are essential for preventing complications and improving long-term health.
Patient Case Study
Allison, a 42-year-old woman, came to my office after months of unexplained hives and nighttime digestive distress. She had visited multiple specialists but received no clear answers. Her symptoms often appeared several hours after dinner, making it difficult for her to identify the cause. After a detailed evaluation, we tested for Alpha-Gal Syndrome, and her results were strongly positive.
Allison was shocked to learn that a tick bite from the previous summer had triggered her symptoms. We began a personalized treatment plan focused on dietary changes, reducing inflammation, and promoting gut healing.
Within weeks, her hives decreased significantly, and her digestion improved. She also reported better sleep and increased energy. Over time, we identified additional food sensitivities that were contributing to her symptoms. With targeted supplements and lifestyle adjustments, her immune system stabilized. Today, Allison feels confident managing her condition and has regained her quality of life. She continues to follow her personalized plan and remains symptom-free.
Why Patients Choose Dr. Dana Cohen for Alpha-Gal Syndrome Treatments
Patients choose me because I take the time to understand their full health story and uncover the root causes of their symptoms. My integrative approach blends the best of conventional and functional medicine for comprehensive care. I use advanced testing to identify hidden triggers and create personalized treatment plans. Patients appreciate my compassionate, patient-centered approach and clear communication.
I focus on long-term healing rather than temporary symptom relief. My protocols are designed to reduce inflammation, restore balance, and support whole‑body wellness. I work collaboratively with patients to ensure they feel empowered and informed. My goal is always to help patients regain control of their health and live with confidence.
Contact Dr. Dana Cohen To Learn More About Alpha-Gal Syndrome Treatments in Manhattan, NYC
Alpha‑Gal Syndrome can be confusing, frightening, and disruptive, but you do not have to navigate it alone. With the right testing and integrative treatment, it is possible to reduce symptoms and restore your quality of life.
My approach focuses on identifying root causes, reducing inflammation, and supporting long-term healing. Whether you are newly diagnosed or still searching for answers, I am here to help.
Together, we will create a personalized plan that fits your needs and lifestyle. You deserve clarity, confidence, and relief from unpredictable reactions. If you are ready to take the next step, I invite you to schedule a consultation. Let’s work together to restore your health and well-being.
Please contact me today!
Additional Information
- Alpha-Gal Syndrome - Centers for Disease Control and Prevention (CDC)
- Tickborne Diseases of the United States - Centers for Disease Control and Prevention (CDC)